Chinese Journal of Tissue Engineering Research ›› 2015, Vol. 19 ›› Issue (4): 531-536.doi: 10.3969/j.issn.2095-4344.2015.04.007
Previous Articles Next Articles
Conservative treatment of mild ossification of cervical posterior longitudinal ligament: prognostic factors and timing of surgical repair
Shen Cang-hai, Feng Yong-jian, Wang Li-guo, Yang Cheng, Peng Ning-ning, Wang Gui-jiang, Guo Xu
- Fourth Department of Orthopedics, Cangzhou Central Hospital, Cangzhou 061001, Hebei Province, China
-
Revised:2014-11-26Online:2015-01-22Published:2015-01-22 -
Contact:Wang Li-guo, Chief physician, Professor, Fourth Department of Orthopedics, Cangzhou Central Hospital, Cangzhou 061001, Hebei Province, China -
About author:Wang Li-guo, Chief physician, Professor, Fourth Department of Orthopedics, Cangzhou Central Hospital, Cangzhou 061001, Hebei Province, China
CLC Number:
Cite this article
Shen Cang-hai, Feng Yong-jian, Wang Li-guo, Yang Cheng, Peng Ning-ning, Wang Gui-jiang, Guo Xu . Conservative treatment of mild ossification of cervical posterior longitudinal ligament: prognostic factors and timing of surgical repair[J]. Chinese Journal of Tissue Engineering Research, 2015, 19(4): 531-536.
share this article
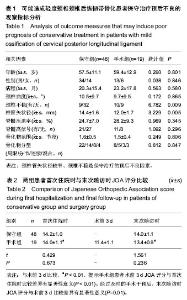
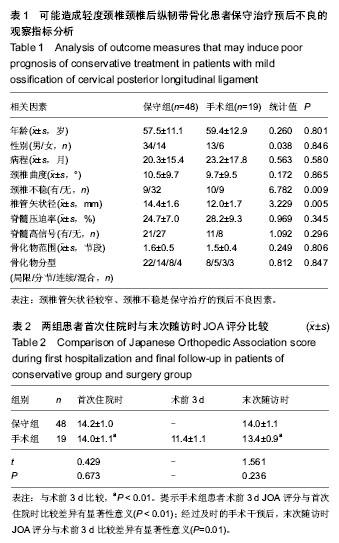
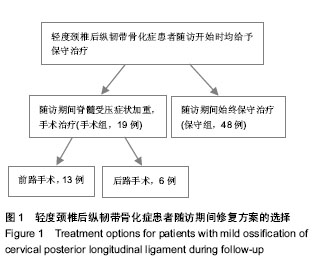
2.1 参与者数量分析 71例轻度颈椎后纵韧带骨化症患者中3例患者失访,1例患者因随访期间创伤致颈髓损伤,其余67例患者获得完整随访,随访时间37-55个月。保守组患者48例随访期间始终接受保守治疗。手术组患者19例保守治疗期间效果不佳,JOA评分平均降低2.7分(2- 5分),接受颈椎前路或后路手术治疗。手术组从随访开始到手术的平均时间27.5个月(19-44个月)。 2.2 保守组与手术组基线资料比较 保守组与手术组患者性别、首次住院时年龄、病程比较差异无显著性意义(P > 0.05),具有可比性(表1)。 2.3 保守治疗的预后因素分析 为了得出保守治疗的预后不良因素,对比保守组与手术组的主要观察指标 (见表1),保守组与手术组颈椎管矢状径差异有显著性意义(t=3.229,P=0.005),手术组患者椎管矢状径明显小于保守组。保守组23%患者颈椎节段不稳,治疗组53%患者颈椎节段不稳,差异有显著性意义(χ2=6.782,P=0.009)。保守组与手术组患者年龄、性别、病程、颈椎曲度、脊髓压迫率、脊髓高信号、骨化物范围、骨化物分型差异均无显著性意义(P > 0.05)。颈椎管矢状径较窄、颈椎不稳是保守治疗的预后不良因素。在保守治疗期间颈椎管矢状径较窄或颈椎不稳的患者往往保守治疗效果不佳,预后不良,最终接受手术治疗。 2.4 保守组与手术组首次住院与末次随访时JOA评分比较 首次住院时保守组与手术组JOA评分差异无显著性意义(t=0.429,P=0.673);末次随访时保守组与手术组JOA评分差异无显著性意义(t=1.561,P=0.236)。手术组患者术前3 d JOA评分为(11.4±1.1)分,术前3 d与首次住院时比较差异有显著性意义(t=5.461,P < 0.01);手术组经过及时的手术干预后,末次随访时JOA评分与术前3 d比较差异有显著性意义(t=4.191,P=0.01,见表2)。"
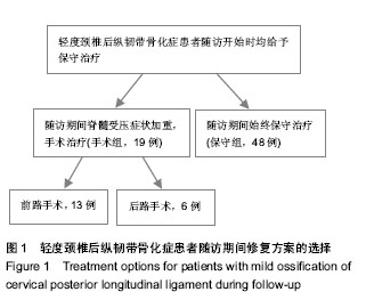
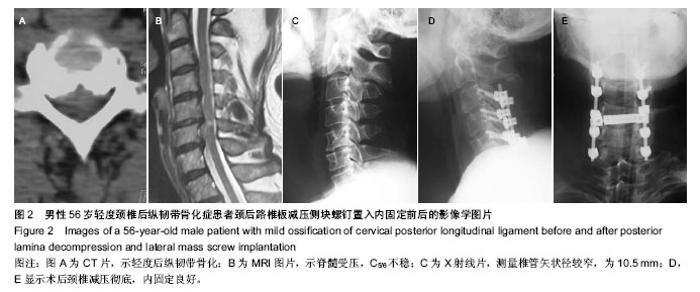
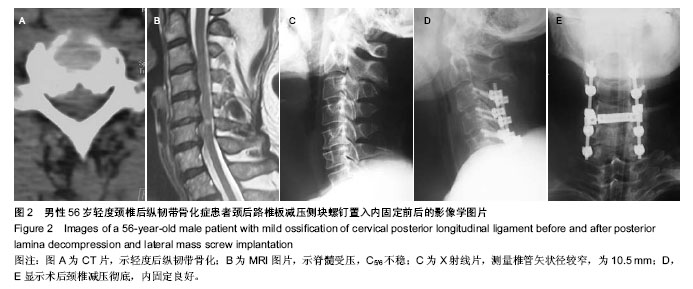
2.5 手术组术中、术后并发症情况 前路减压13例,采用骨化块切除或漂浮植骨融合内固定。4例采用后路单开门椎管成形,2例术前存在颈椎曲度后凸畸形的患者采用后路椎板减压侧块螺钉内固定。手术组中前路手术并发症包括1例脑脊液漏。后路手术并发症包括1例C5神经根麻痹和2例颈肩部的轴性痛。前路脑脊液漏患者均因骨化物与硬膜囊粘连紧密,分离、切除骨化物时撕裂硬膜囊,经局部压迫并平卧3-5 d脑脊液漏停止。C5神经根麻痹发生在术后纠8 h内,予以口服神经营养药物及功能锻炼等保守治疗,术后2个月肌力恢复至4级。颈肩部轴性痛患者给予口服非类固醇抗炎药缓解疼痛,术后3个月疼痛逐渐消失。 2.6 典型病例 男性患者,56岁,首次入院时JOA评分为14分。患者存在保守治疗预后不良因素,随访期间保守治疗效果不佳,JOA评分降为11分。行颈后路椎板减压侧块螺钉置入内固定,术后末次随访时JOA评分为13分,修复效果良好,见图2。"
| [1] Yoshii T, Yamada T, Hirai T, et al. Dynamic changes in spinal cord compression by cervical ossification of the posterior longitudinal ligament evaluated by kinematic computed tomography myelography. Spine (Phila Pa 1976). 2014;39(2): 113-119. [2] Fujimori T, Iwasaki M, Okuda S, et al. Long-term results of cervical myelopathy due to ossification of the posterior longitudinal ligament with an occupying ratio of 60% or more. Spine (Phila Pa 1976). 2014;39(1):58-67. [3] Izumi T, Hirano T, Watanabe K, et al. Three-dimensional evaluation of volume change in ossification of the posterior longitudinal ligament of the cervical spine using computed tomography. Eur Spine J. 2013;22(11):2569-2274. [4] 贾连顺.颈椎后纵韧带骨化并不都需要手术[J]. 中国矫形外科杂志, 2009,17(7): 47-49. [5] Sah S, Wang L, Dahal M, et al. Surgical management of cervical spondylotic myelopathy. J Nepal Med Assoc. 2012; 52(188):172-177. [6] Pham MH, Attenello FJ, Lucas J, et al. Conservative management of ossification of the posterior longitudinal ligament. A review. Neurosurg Focus. 2011;30(3):E2. [7] Matsunaga S, Sakou T, Taketomi E, et al. The natural course of myelopathy caused by ossification of the posterior longitudinal ligament in the cervicalspine. Clin Orthop Relat Res. 1994; 8(305):168-177. [8] Matsumoto M, Toyama Y, Ishikawa M, et al. Increased signal intensity of the spinal cord on magnetic resonance images in cervical compressive myelopathy. Does it predict the outcome of conservative treatment? Spine (Phila Pa 1976). 2000;25(6): 677-682. [9] Wilson JR, Barry S, Fischer DJ, et al. Frequency, timing, and predictors of neurological dysfunction in the nonmyelopathic patient withcervical spinal cord compression, canal stenosis, and/or ossification of the posterior longitudinal ligament.Spine (Phila Pa 1976).2013;38(22 Suppl 1):S37-54. [10] Mochizuki M, Aiba A, Hashimoto M, et al. Cervical myelopathy in patients with ossification of the posterior longitudinal ligament. J Neurosurg Spine. 2009;10(2): 122-128. [11] Wu JC, Liu L, Chen YC, et al. Ossification of the posterior longitudinal ligament in the cervical spine: an 11-year comprehensive national epidemiology study. Neurosurg Focus. 2011;30(3):E5. [12] Xing D, Wang J, Ma JX, et al. Qualitative evidence from a systematic review of prognostic predictors for surgical outcomes followingcervical ossification of the posterior longitudinal ligament. J Clin Neurosci. 2013;20(5):625-633. [13] Li H, Jiang LS, Dai LY. A review of prognostic factors for surgical outcome of ossification of the posterior longitudinal ligament ofcervical spine. Eur Spine J. 2008; 17(10): 1277-1288. [14] Hyun SJ, Riew KD, Rhim SC. Range of motion loss after cervical laminoplasty: a prospective study with minimum 5-year follow-up data. Spine J. 2013;13(4):384-390. [15] Matsuyama Y, Kawakami N, Yanase M, et al. Cervical myelopathy due to OPLL: clinical evaluation by MRI and intraoperative spinal sonography. J Spinal Disord Tech. 2004; 17(5):401-404. [16] Vedantam A, Jonathan A, Rajshekhar V. Association of magnetic resonance imaging signal changes and outcome prediction after surgery forcervical spondylotic myelopathy. J Neurosurg Spine. 2011;15(6):660-666. [17] Kimura A, Seichi A, Hoshino Y, et al. Perioperative complications of anterior cervical decompression with fusion in patients with ossification of the posterior longitudinal ligament: a retrospective, multi-institutional study. J Orthop Sci. 2012;17(6):667-672. [18] Fujimori T, Iwasaki M, Nagamoto Y, et al. Three-dimensional measurement of intervertebral range of motion in ossification of the posterior longitudinal ligament: are there mobile segments in the continuous type? J Neurosurg Spine. 2012;17(1):74-81. [19] Odate S, Shikata J, Kimura H, et al. Anterior corpectomy with fusion in combination with an anterior cervical plate in the management of ossification of the posterior longitudinal ligament. J Spinal Disord Tech. 2012;25(3):133-137. [20] Nakamura K, Kurokawa T, Hoshino Y, et al. Conservative treatment for cervical spondylotic myelopathy: achievement and sustainability of a level of “no disability”. J Spinal Disord. 1998;11(2):175-179. [21] Epstein N. Posterior approaches in the management of cervical spondylosis and ossification of the posterior longitudinal ligament. Surg Neurol. 2002;58(3-4):194-208. [22] 陈德玉.颈椎后纵韧带骨化症的治疗现状[J].中国脊柱脊髓杂志, 2010, 20(3):181-183. [23] Sun Q, Hu H, Zhang Y, et al. Do intramedullary spinal cord changes in signal intensity on MRI affect surgical opportunity and approach for cervical myelopathy due to ossification of the posterior longitudinal ligament? Eur Spine J. 2011;20(9): 1466-1473. [24] Yonenobu K. Is surgery indicated for asymptomatic or mildly myelopathic patients with significant ossification of the posterior longitudinal ligament? Spine (Phila Pa 1976). 2012; 37(5):E315-317. [25] Tsuyama N. Ossification of the posterior longitudinal ligament of the spine. Clin Orthop Relat Res. 1984; (184):71-84. [26] Harsh GR 4th, Sypert GW, Weinstein PR, et al. Cervical spine stenosis secondary to ossification of the posterior longitudinal ligament. J Neurosurg. 1987;67(3):349-357. [27] Nurick S. The pathogenesis of the spinal cord disorder associated with cervical spondylosis. Brain. 1972;95(1):87-100. [28] 陈宇,陈德玉,王新伟,等.严重颈椎后纵韧带骨化症前路和后路手术比较[J].中华骨科杂志,2008, 28(9):705-709. [29] 申勇,王林峰,张英泽,等. MRI信号强度及临床表现对判断颈椎后纵韧带骨化症预后的作用[J].中华骨科杂志, 2009, 29(3): 212-215. [30] Ogawa Y, Chiba K, Matsumoto M, et al. Long-term results after expansive open-door laminoplasty for the segmental-type of ossification of the posterior longitudinal ligament of the cervical spine: a comparison with nonsegmental-type lesions. J Neurosurg Spine. 2005;3(3): 198-204. [31] Choi S, Lee SH, Lee JY, et al. Factors affecting prognosis of patients who underwent corpectomy and fusion for treatment of cervical ossification of the posterior longitudinal ligament: analysis of 47 patients. J Spinal Disord Tech. 2005;18(4): 309-314. [32] Oshima Y, Seichi A, Takeshita K, et al. Natural course and prognostic factors in patients with mild cervical spondylotic myelopathy with increased signal intensity on T2-weighted magnetic resonance imaging. Spine (Phila Pa 1976). 2012; 37(22):1909-1913. |
| [1] | Chen Qun-qun, Qiao Rong-qin, Duan Rui-qi, Hu Nian-hong, Li Zhao, Shao Min. Acu-Loc®2 volar distal radius bone plate system for repairing type C fracture of distal radius [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(7): 1025-1030. |
| [2] | Zou Wei, Xiao Jie, Long Hao, Zhang Yang, Wu Chen, Du Yu-hui, Feng Ming-xing, Zhou Chang-jun. Screw placement selection of minimally invasive percutaneous pedicle screw fixation for thoracolumbar fractures [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 356-361. |
| [3] | Chen Lu-yao, Hu Shi-qiang, Wang Xiao-ping, Wu Wei-wei, Wei Zhan-tu, Huang Jian. Accuracy of digital orthopedic three-dimensional reconstruction for thoracolumbar pedicle screw placement [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 373-377. |
| [4] | Du Shi-yao, Zhou Feng-jin, Ni Bin, Chen Bo, Chen Jin-shui. Finite-element analysis of a novel posterior atlantoaxial restricted non-fusion fixation system [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 383-389. |
| [5] | Liu Jun, Liao Su-ping. Three-dimensional finite element analysis of Kirschner nails and external fixation for Bennett fracture [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 390-395. |
| [6] | Sheng Xiao-lei, Yuan Feng, Li Zhi-duo, Yang Yu-ming, Lu Hai-tao, Zhang Jun-wei. Comparison of the accuracy of lower cervical anterior transpedicular screws between three-dimensional printing assembly navigation template and free hand placement [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 406-411. |
| [7] | Wang Xing, Zhang Shao-jie, Shi Jun, Li Xiao-he, Liu Ying, Li Zhi-jun, Hou Er-fei, Chen Jie, Wang Wei. Correlation of uncinate process and various vertebral body structures in adolescents: three-dimensional reconstruction based on CT images [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 412-417. |
| [8] | Wu Min-hao, Sun Wen-chao, Yan Fei-fei, Xie Yuan-long, Hou Zhi-qiang, Feng Fan, Cai Lin . Treatment research and new progress of early-onset scoliosis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 433-439. |
| [9] | Wang Lei, Wang Feng-feng, Ma Yan-hui, Zhang Jie, Hu Fang, Ma Gai-ping, Liu Mei-mei, Ma Zhang-wen. Meta analysis of clinical outcome of intramedullary nails versus locking plates for two-part proximal humerus fracture [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(3): 478-484. |
| [10] | Hu Jun, Zhang De-qiang, Tang Xin. Postoperative quality of life of internal fixation versus hemiarthroplasty for femoral neck fractures in the elderly [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(19): 2953-2960. |
| [11] | Jiang Wei, Yuan Feng. Unilateral pedicle screw fixation combined with translaminar facet screw fixation versus bilateral pedicle screw fixation for lower lumbar degenerative diseases: a 2-year follow-up [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(19): 2973-2979. |
| [12] | Wang Xiu-ping, Sun Rui-bo, Liu You-wen, Zhang Ying, Jia Yu-dong, Yang Yu-xia, Wang Hui-chao. Femoral neck fractures fixed with intramedullary cannulated screws: factors for postoperative functional recovery [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(19): 2999-3004. |
| [13] | Liu Gang, Zhang Lei, Wang Guo-you, Zhou Xin, Zhang Tao, Guan Tai-yuan, Guo Xiao-guang, Fu Shi-jie. Double-row suture anchors under arthroscopy for avulsion-type greater tuberosity fractures (Mutch type I) [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(19): 3005-3010. |
| [14] | Yang Min, Ma Xiang-yang, Yang Jin-cheng, Chen Shu-jin, Zou Xiao-bao. Biomechanical properties of a novel automatic anti-rotation posterior atlantoaxial internal fixation system: a finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2017, 21(19): 3031-3037. |
| [15] | Qiu Hao, Lu Min-peng, Dong Jing, Zhang Zhong-zu, Chu Tong-wei, Wang Qun-bo, Quan Zheng-xue, Jiang Dian-ming. Subtotal corpectomy and reconstruction with titanium mesh cage implantation and pedicle screw fixation through posterior approach in treatment of thoracolumbar burst fracture or thoracolumbar fracture dislocation [J]. Chinese Journal of Tissue Engineering Research, 2016, 20(53): 7932-7938. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||